Symptoms, Causes, and Natural Treatments for IBS

Dr. Derek Cook has a background in biology and chemistry and training in Auricular medicine. He takes an aggressive approach to provide fast results. He focuses on individualized care using core health fundamentals and bioenergetic assessment to support lasting healing.
View full profile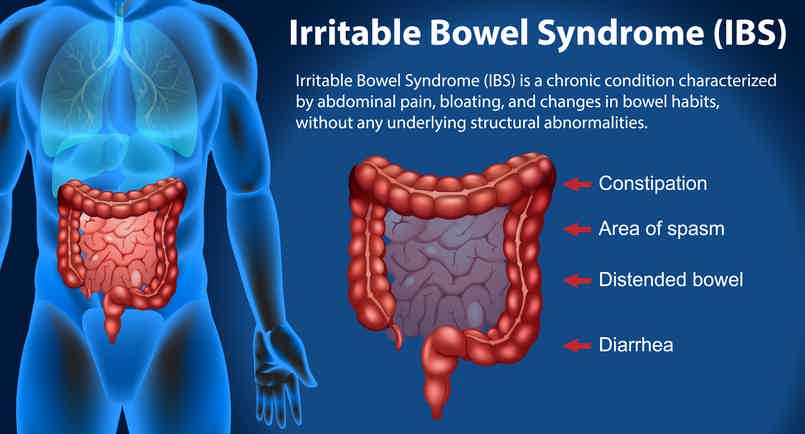
Irritable Bowel Syndrome (IBS) is one of the most common digestive concerns seen in clinical practice—yet for many people, it remains a confusing and frustrating diagnosis. IBS affects an estimated 10–20% of the population at any given time, with women seeking care more often than men.
Although IBS is extremely common, symptoms differ from person to person, and the root causes vary widely. As a result IBS symptoms can be experienced in a highly personal way, suffering in their own unique way and can be very different from one another.
If you struggle with bloating, abdominal discomfort, constipation, diarrhea, food reactions, or ongoing digestive instability, understanding IBS is the first step toward finally getting relief.
This guide breaks down what IBS actually is, the many symptoms it can cause, and the treatment approaches proven helpful according to the provided research and clinical experience.
What Is IBS?
IBS is defined as a functional disorder of the large intestine, meaning symptoms occur without visible structural disease. People with IBS experience combinations of:
Abdominal pain
Constipation and/or diarrhea
Gas, bloating, nausea, and mucus in stool
Digestive discomfort after eating
IBS is often referred to as a diagnosis of exclusion—other causes such as celiac disease, inflammatory bowel disease (Crohn’s and Ulcerative Colitis), infections, and malabsorption must be ruled out before IBS can be confirmed.
Importantly, IBS is not caused by one single issue. IBS is essentially “a label for a set of symptoms” with hundreds of possible causes, and the real work lies in identifying the individual triggers.
What are the Common Symptoms of IBS?
Abdominal Pain is a hallmark IBS symptom and often improves with a bowel movement.
Bloating may feel like pressure, sponginess, hardness, or visible abdominal distension—it isn’t always due to excess gas. Mechanisms include distension, increased visceral sensitivity, altered motility, and abdominal wall muscle changes.
Constipation, Diarrhea, or Both. IBS may present as:
IBS-C (constipation predominant), very common in Small Intestinal Bacterial Overgrowth (SIBO). More than 25% of bowel movements are hard and lumpy.
IBS-D (diarrhea predominant). More than 25% of bowel movements are loose and watery.
IBS-M (mixed). More than 25% of bowel movements are hard and lumpy, and more than 25% are loose and watery.
IBS-U (unsubtyped). Unclassified and don’t fit any of the above subtypes
Gas and Flatulence. Many patients report ongoing gas, burping, or digestive discomfort, sometimes driven by food intolerances, dysbiosis, or FODMAP sensitivity.
Extraintestinal Symptoms. Research shows IBS frequently coexists with:
Fatigue
Headaches and migraines
Sleep disturbances
Irritable bladder
Restless legs syndrome (RLS)
Dyspareunia (painful intercourse)
What Causes IBS? Understanding Key Triggers
Food Allergies or Intolerances
Research shows up to two-thirds of IBS patients have at least one food intolerance. Common reactive foods include dairy, wheat and grains, yeast, eggs, soy, beef, and foods high in sugar.Dysbiosis or Small Intestinal Bacterial Overgrowth (SIBO)
SIBO occurs when bacteria overgrow in the small intestine, causing fermentation, gas, and inflammation. Key symptoms include bloating, gas, abdominal pain, constipation or diarrhea, burping, and distention.FODMAP Sensitivities
FODMAPs are fermentable carbohydrates that worsen symptoms. Research suggests 75% of IBS patients improve on a low-FODMAP diet. However, in my clinic experience, not addressing the underlying dysbiosis (imbalance of the gut microbiome) can result in a Fodmap diet being a management tool rather than a path to sustainable health. This emphasizes the need to treat the underlying cause.Stress, Anxiety, and the Brain–Gut Axis
Stress can trigger gut spasms, increase or decrease motility, heighten pain sensitivity, alter the gut microbiome and reduce immune function.Sugar and Processed Foods
Meals high in refined sugar slow intestinal motility and promote bacterial overgrowth, promote fungal overgrowth such as Small Intestinal Fungal Overgrowth (SIFO), alter the gut microbiome (SIBO) and create leaky gut (intestinal hyperpermeability), the guts natural physical barrier breaks down allowing harmful substances like toxins, bacteria and partially digested food particles to pass into the bloodstream.
How IBS Is Diagnosed? A thorough assessment includes:
Full history and physical exam
Blood work
Food Sensitivity Test (FST) and/or Food elimination and re-introductory
Celiac screening
Stool testing
Breath testing for SIBO
Endoscopy or colonoscopy to exclude polyps, ulcers and other structural issues
What are the Evidence-Based Treatment Approaches for IBS?
Dietary Strategies. Increase non-allergenic fiber such as fruit/vegetable fiber and PHGG. Potentially follow a low-FODMAP diet. Food elimination and re-introductory to identify possible food intolerances, this can be aided with a Food Sensitivity Test.
Treat Dysbiosis and SIBO. Herbal antimicrobials, probiotics, dietary changes, antibiotics like rifaximin and motility agents like ginseng and prucalopride micro dosing.
Probiotics. Strains such as Bifidobacterium infantis and Lactobacillus rhamnosus may help. If dealing with SIBO, probiotics are initially restricted to spore based probiotics.
Botanical Medicine. Thyme, Golden Seal, Myrrh and Robert’s formula, a traditional herbal used effectively for over 300 years in the treatment of IBS.
Mind–Body and Lifestyle Therapies. This includes diet modifications, good sleep hygiene, good movement/exercise and stress management strategies including a biofeedback technique, Auricular Bioenergetic Medicine.
Final Thoughts
IBS is real, impactful, and multifactorial—but highly treatable when underlying triggers are identified. If you’re struggling with bloating, pain, or unpredictable digestion, we’re here to help. Connect with us to explore your personalized treatment options.
Ready to get started?
Book your free discovery call with a Naturopathic Doctor of your choice.
Free Discovery CallDisclaimer: The information in this blog is for educational purposes only and does not replace professional medical advice. Always consult a qualified healthcare provider with questions regarding your health.
