Perimenopause Symptoms Checklist and Natural Hormone Support

Are you dismissing those sudden mood swings and brain fog as "just stress"? If you're over 35 and experiencing unexplained anxiety or irregular periods, your body might be sending you important signals about perimenopause that you shouldn't ignore.
Key Takeaways
Perimenopause typically begins around age 46, though some women notice changes as early as their mid-30s or as late as their mid-50s, with irregular periods often being the first warning sign
Eight key symptoms include hot flashes, sleep disturbances, mood changes, brain fog, and anxiety—all linked to declining estrogen levels
Hormone therapy benefits may outweigh risks when started before age 60 or within 10 years of menopause, using the lowest effective dose
Natural management strategies including weight-bearing exercise, stress reduction, and evidence-based supplements can significantly reduce symptom severity
Understanding when symptoms require medical attention helps women make informed decisions about their perimenopause journey
The transition into perimenopause can feel overwhelming, especially when symptoms seem to appear suddenly or intensify without warning. Many women wonder if what they’re experiencing is simply part of the transition or something that deserves attention. If your symptoms are starting to impact your daily life, consider seeking professional guidance because you don’t have to navigate this alone. This guide provides a clear checklist of perimenopause symptoms and practical guidance on when hormone support might be beneficial for your unique situation.
Think of your hormones as a long-standing weather pattern. For most of your reproductive years, the forecast is fairly predictable.You know the rhythm of the seasons and how your body typically responds. But during perimenopause, that familiar weather system starts to shift.
Some days bring sudden heat, like unexpected warm fronts that rise out of nowhere and leave you flushed and uncomfortable. Other days feel like passing storms, with mood changes or irritability rolling in and out without warning. There may be stretches of calm followed by abrupt changes in energy, sleep, or cycle length much like waking up to a completely different forecast than the day before.
The climate itself hasn’t changed; your body is simply transitioning into a new pattern. And just like adapting to evolving weather, learning what supports you through these fluctuations can make the entire transition feel more manageable and predictable.
Are You Experiencing These 8 Key Perimenopause Warning Signs?
Perimenopause announces itself differently for each woman, but certain warning signs consistently appear across most experiences. The most common early indicator is irregular menstrual cycles—periods may become shorter or longer, heavier or lighter, or arrive unpredictably. This happens because your ovaries begin producing less estrogen, typically starting around age 46, though some women notice changes as early as their mid-30s or as late as their mid-50s.
Hot flashes rank as the second most recognizable sign, affecting nearly 80% of women worldwide who suffer from vasomotor symptoms. These sudden waves of heat, often accompanied by sweating and a flushed face, can last from seconds to several minutes. Sleep disturbances frequently follow, with many women experiencing insomnia or night sweats that disrupt restorative sleep patterns.

Mood changes represent another significant warning sign that shouldn't be dismissed. Many women report increased irritability, anxiety, or mood swings that seem disproportionate to life circumstances. The naturopathic doctors at Healthflow Naturopathic recognizes these emotional shifts as valid symptoms that deserve proper attention and support during this transitional phase.
The remaining warning signs include brain fog (difficulty concentrating or remembering), decreased libido, vaginal dryness, weight gain (particularly around the midsection), and joint aches. Recognizing these patterns early helps women understand they're not alone and that effective management strategies exist.
Complete Perimenopause Symptoms Checklist
1. Physical Changes You'll Notice First
Physical symptoms often provide the clearest evidence that perimenopause has begun. Beyond irregular periods, many women notice changes in menstrual flow—periods may become significantly heavier with large clots, or conversely, much lighter than usual. Some experience breakthrough bleeding between cycles or after intercourse.
Temperature regulation problems extend beyond classic hot flashes. Many women become more sensitive to temperature changes, feeling uncomfortably warm in previously comfortable environments. Night sweats can be particularly disruptive, leading to frequent awakening and the need to change clothing or bedding.
Physical discomfort manifests in various ways: headaches may become more frequent or intense, joint stiffness increases (especially in the morning), and breast tenderness can occur even when periods are irregular. Weight distribution often shifts, with fat accumulating around the waist despite unchanged eating or exercise habits.
2. Mental and Emotional Shifts That Signal Transition
The connection between declining estrogen and mental health changes is well-established. Low estrogen levels reduce serotonin production, which can increase irritability, anxiety, and feelings of sadness. These aren't character flaws or signs of weakness—they're biological responses to hormonal fluctuations.
Cognitive changes frequently accompany emotional shifts. Many women describe feeling "foggy" or having difficulty finding words they know well. Memory lapses become more common, and concentration requires more effort than before. These symptoms can be particularly frustrating for women accustomed to mental sharpness.
Anxiety symptoms may appear for the first time or worsen if already present. This can include racing thoughts, physical tension, difficulty relaxing, or unexpected worry about routine situations. Sleep problems often compound these issues, creating a cycle where poor rest worsens emotional regulation.
3. When Symptoms Require Medical Attention
While many perimenopause symptoms are normal, certain signs warrant prompt medical evaluation. Extremely heavy bleeding that requires soaking through one or more pads or tampons every hour for several consecutive hours needs immediate attention. Similarly, if bleeding lasts longer than seven days, it may mean there's an issue with your reproductive health that needs diagnosis and treatment.
If periods are usually less than 21 days apart, it may mean there's an issue with your reproductive health that needs diagnosis and treatment. Additionally, if you have gone 12 months without a period and then start bleeding, tell your healthcare professional, as you could have a health issue.
Severe mood changes that interfere with daily functioning, relationships, or work performance deserve professional support. This includes persistent feelings of depression, overwhelming anxiety, or thoughts of self-harm. These symptoms may indicate clinical depression or anxiety disorders that require specific treatment beyond hormone support.
Understanding Your Hormone Changes During Perimenopause
Why Estrogen Decline Triggers These Symptoms
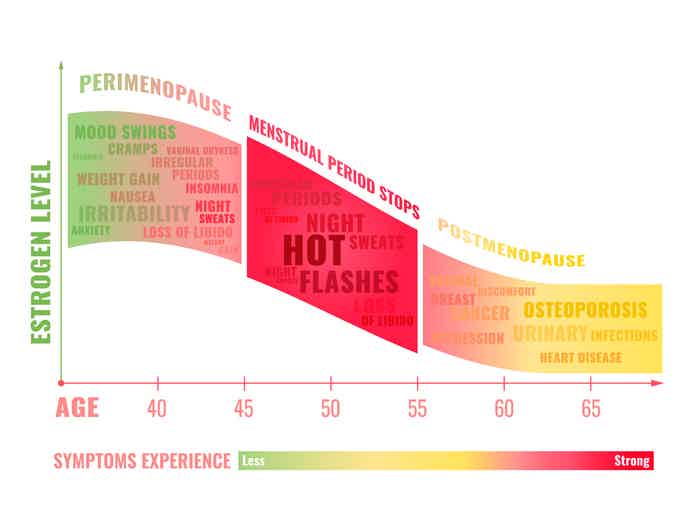
Estrogen serves far more functions than supporting reproduction. This hormone helps regulate body temperature, supports bone density, influences mood neurotransmitters, and maintains vaginal tissue health. As estrogen levels fluctuate and gradually decline, each of these systems experiences disruption, creating the wide-ranging symptoms women experience.
The hypothalamus, your body's temperature control center, becomes less effective at regulating heat when estrogen drops. This explains why minor temperature changes can trigger intense hot flashes or why you might feel cold one moment and overheated the next.
Estrogen also influences how your body processes and stores fat. Lower levels promote fat storage around the abdomen rather than hips and thighs, contributing to the weight distribution changes many women notice during perimenopause.
The Connection Between Low Estrogen and Anxiety
The relationship between estrogen and emotional well-being runs deeper than many realize. Omega-3s, particularly DHA, support brain health and help improve mood by enhancing the function of your brain chemicals (neurotransmitters like serotonin and dopamine) which can help improve depression, anxiety and irritability.
Serotonin deficiency linked to low estrogen can manifest as increased worry, difficulty enjoying previously pleasant activities, or feeling emotionally "flat." Many women describe feeling less resilient to stress or finding that minor irritations feel overwhelming.
The gut-brain connection also plays a role, as estrogen influences digestive function and the gut microbiome. Changes in gut health during perimenopause can further impact mood and anxiety levels, creating a complex web of interconnected symptoms.
How Hormonal Changes Increase Vulnerability to Emotional Disturbance
Hormonal fluctuations during perimenopause don't just cause direct symptoms—they also reduce your body's ability to cope with stress. The same life challenges that you previously managed well may suddenly feel overwhelming or unmanageable.
Sleep disruption compounds emotional vulnerability. Poor sleep quality, whether from night sweats, anxiety, or other perimenopause symptoms, reduces emotional regulation abilities and increases reactivity to stressful situations.
Blood sugar fluctuations often worsen during perimenopause due to hormonal changes, contributing to mood swings, energy crashes, and irritability. Understanding these connections helps women recognize that their emotional experiences have biological roots requiring appropriate support.
When to Consider Hormone Therapy Support
1. Symptoms That Respond Best to Hormone Therapy
Vasomotor symptoms—hot flashes and night sweats—show the most dramatic improvement with hormone therapy. Studies consistently demonstrate that menopausal hormone therapy (MHT) provides the most effective relief for these temperature regulation problems, often reducing frequency and intensity by 80-90%.
Genitourinary symptoms including vaginal dryness, painful intercourse, and urinary urgency respond excellently to hormone therapy. These symptoms often worsen without treatment and can significantly impact quality of life and intimate relationships.
Sleep disturbances related to night sweats or hormonal fluctuations typically improve with hormone support. Better sleep quality creates positive cascading effects on mood, energy levels, and overall well-being.
2. Optimal Timing: Before Age 60 and Within 10 Years of Menopause
Timing matters significantly for hormone therapy safety and effectiveness. Research indicates that the benefits of menopause hormone therapy may outweigh the risks if treatment is started before age 60 or within 10 years of the final menstrual period. Starting within this "window of opportunity" provides maximum benefits while minimizing risks.
Early initiation during perimenopause or early menopause may help prevent some long-term health issues including bone loss and cardiovascular changes. Women who start hormone therapy later in life face increased risks without receiving the same protective benefits.
Individual assessment remains crucial, as personal health history, family history, and current symptoms all influence whether hormone therapy is appropriate and when to begin treatment.
3. Using Lowest Effective Dose for Shortest Time Needed
Modern hormone therapy protocols emphasize individualized dosing that provides symptom relief while minimizing exposure. This approach often involves starting with lower doses and adjusting based on symptom response rather than using standardized doses for all women.
Transdermal delivery methods (patches, gels, creams) often allow for lower doses compared to oral medications while providing effective symptom control. These methods also avoid the "first-pass" effect through the liver, potentially reducing certain risks.
Regular monitoring helps ensure women receive ongoing benefits without unnecessary exposure. Many women find they can reduce doses over time as symptoms naturally improve or use hormone therapy intermittently rather than continuously.
4. Understanding Risks: Heart Disease Considerations for Older Women
Age at initiation significantly influences cardiovascular risks associated with hormone therapy. Women who start hormone therapy after age 60 or more than 10 years past menopause face increased risks of heart disease, stroke, and blood clots compared to younger initiators.
Pre-existing cardiovascular risk factors require careful consideration. Women with a history of heart disease, stroke, blood clots, or multiple cardiovascular risk factors may not be suitable candidates for systemic hormone therapy.
The benefits of HRT typically outweigh risks when started before age 60 in healthy women. However, individual risk-benefit analysis should always guide treatment decisions, considering personal health history and symptom severity.
5. Alternative Options Beyond Hormone Therapy
Non-hormonal medications can effectively manage specific perimenopause symptoms. Certain antidepressants help with hot flashes and mood symptoms, while gabapentin can reduce hot flash frequency and improve sleep quality.
Bioidentical hormones represent another option, though scientific evidence supporting advantages over conventional hormone therapy remains limited. These compounds have identical molecular structure to human hormones but require the same careful consideration of risks and benefits.
Combination approaches often work best, integrating medical treatments with lifestyle modifications and natural support strategies to address symptoms from multiple angles.
Natural Ways to Manage Perimenopause Symptoms
Lifestyle Changes: Weight Management and Regular Exercise

Studies that involve providing exercise alongside protein (through diet or supplements), vitamin D and calcium showed reduced risk for falls, fractures, reduced sarcopenia scores, and increased muscle mass and strength.
Activities like walking, hiking, dancing, or strength training for 150 minutes per week can significantly reduce symptom severity. Protecting your muscle mass during perimenopause and into later life is one of the most impactful investments you can make in your long-term health, energy, and resilience.
Maintaining healthy weight becomes more challenging during perimenopause due to metabolic changes, but it's crucial for overall symptom management. Even modest weight loss can reduce hot flash frequency and intensity while improving energy levels.
Consistent meal timing helps stabilize blood sugar and energy levels. Eating balanced meals with adequate protein every 3-4 hours can reduce mood swings, energy crashes, and food cravings that often worsen during hormonal transitions.
Stress Reduction Techniques: Meditation and Aromatherapy
Mind-body practices like yoga, meditation, or tai chi show significant benefits for perimenopause symptoms. These activities can improve both physical symptoms like hot flashes and emotional symptoms including anxiety and mood swings.
Deep breathing techniques specifically help manage hot flashes when they occur. Slow, deliberate breathing can reduce hot flash intensity and duration while providing immediate stress relief during challenging moments.
Sea buckthorn oil has been studied for its potential uses in vaginal dryness, and in one study, it showed beneficial effects on vaginal health. While research is limited, many women report improved sleep, reduced anxiety, and better mood with regular aromatherapy use.
Evidence-Based Natural Supplements
While some studies have shown positive effects of black cohosh, others have found it to have little to no use in treating symptoms of menopause. Individual responses vary significantly among herbal supplements for perimenopause symptoms.
Omega-3 fatty acids are essential nutrients that support your heart health, cognitive function, mood stability, joint health and help inflammation too – issues which can all be affected by hormone changes during perimenopause and menopause. High-quality fish oil supplements providing 1-2 grams of EPA and DHA daily can be beneficial for many women.

Adequate vitamin D and calcium intake is the cornerstone of osteoporosis prevention and treatment. Most women require supplementation to achieve optimal levels, especially if dietary intake is insufficient or sun exposure is limited.
Take Control of Your Perimenopause Journey Today
Understanding perimenopause symptoms and treatment options empowers women to make informed decisions about their health during this significant life transition. Whether choosing hormone therapy, natural approaches, or combination strategies, the key lies in working with qualified healthcare providers who understand the complexity of this hormonal shift.
Early recognition and proactive management can significantly improve quality of life during perimenopause. Many women find that addressing symptoms promptly prevents them from worsening and helps maintain their sense of well-being throughout the transition.
Individual approaches work best because perimenopause affects each woman differently. What works well for one woman may not suit another, making personalized assessment and treatment planning essential for optimal outcomes.
Remember that perimenopause is a normal life stage, not a medical condition requiring treatment, but uncomfortable symptoms deserve attention and support. The transition may last several years, but with proper understanding and management, women can navigate this phase while maintaining their health, energy, and quality of life.
For perimenopause support and personalized treatment options, Healthflow Naturopathic provides patient-first naturopathic care to help women navigate their unique hormonal transitions.
Ready to get started?
Book your free discovery call with a Naturopathic Doctor of your choice.
Free Discovery CallDisclaimer: The information in this blog is for educational purposes only and does not replace professional medical advice. Always consult a qualified healthcare provider with questions regarding your health.
